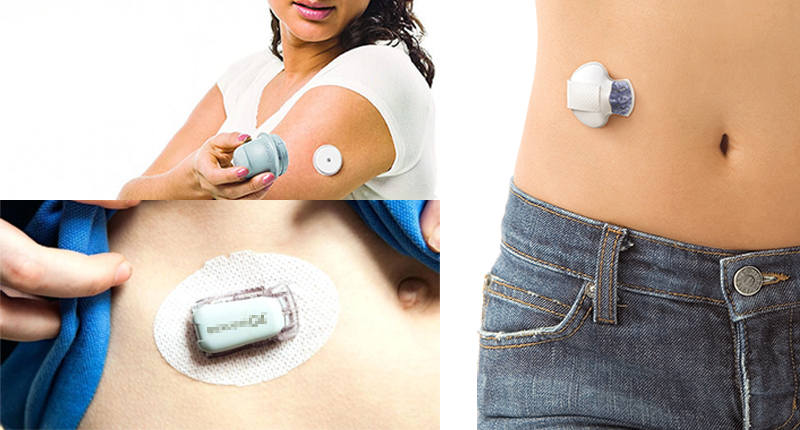
What is a continuous blood glucose meter (CGM)?
CGM is an abbreviation for Continuous Glucose Monitor, which is a device that measures blood sugar levels continuously and helps to manage blood sugar.
With a normal glucose monitor, it is difficult to identify a trend and frequent blood tests are required, which is not as helpful in managing blood sugar levels.
With a cgm, blood sugar levels and trends can be seen in real time, so it is easier to cope with hypoglycemia and hyperglycemia in advance. It can also help to reduce the ups and downs of blood sugar, as trends can be identified earlier. This allows for blood sugar management at a more constant level and trend.
Components of a CGM
The Sensor
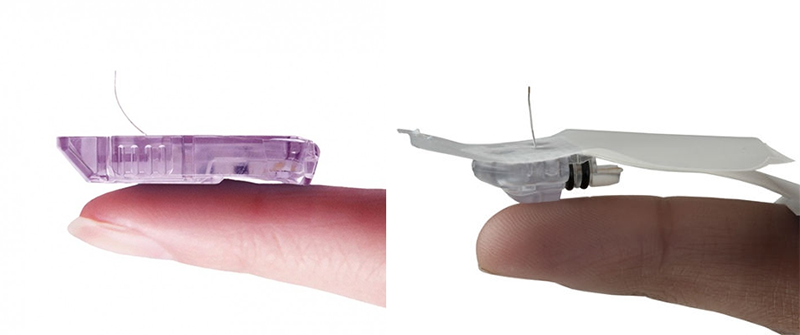
The sensor is a component that sits on the skin, with a small string inserted into the skin via a needle.
It measures blood sugar levels through the interstitial fluid between the cells.
The Transmitter

The transmitter is responsible for sending the blood sugar levels measured by the sensor at regular intervals.
For most cgms, the transmitter and the sensor are a set that need to be used together.
The Receiver

The receiver is a component that reads the blood sugar levels sent by the transmitter and displays the value to the user.
These days, it is also possible to install an app on a smartphone or smartwatch and use them as a receiver.
Wearing a CGM